What Is Respiratory Distress Syndrome (RDS)?
Respiratory Distress Syndrome, or RDS, is a breathing disorder that affects newborn babies, most commonly those who are born preterm—6 weeks or more before their due date. RDS usually develops within the first 24 hours after birth and requires a medical diagnosis. The more premature the baby, the more likely he or she is to have RDS and to need breathing support.1
Babies showing symptoms of RDS are likely to be moved to a neonatal intensive care unit (NICU), where they can receive individualized care based on their specific needs. A baby with RDS may need breathing support and, depending on several factors, treatment can include oxygen therapy and other forms of therapy that may assist with breathing.2 Typically, RDS will worsen over the first 48 to 72 hours after birth and then improve with treatment.3
The History of RDS: A Look Inside the Kennedy Story4
In 1963, John F. Kennedy and his wife Jackie lost their premature son, Patrick, at the age of only 39 hours after he was diagnosed with hyaline membrane disease, also known as RDS. Unfortunately, the loss experienced by the Kennedys was shared by many other families at that time, with 25,000 premature babies diagnosed with RDS and 10,000 dying each year. However, the event marked the beginning of an explosion of research and funding into the causes and management of prematurity. Today’s numbers tell a much different story, as RDS has a much better prognosis with medical intervention. Thanks to an array of treatment options, most premature babies diagnosed with RDS recover from it, and many born much earlier and smaller than the President’s son have a remarkably good chance of surviving.
What Causes RDS?
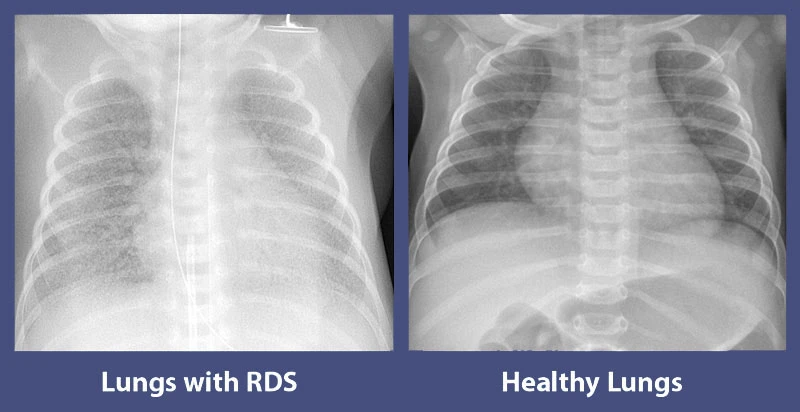
RDS occurs when a baby’s lungs do not make enough surfactant—a slippery liquid substance produced by the lungs to keep the airways (or more specifically, the alveoli, which are the tiny air sacs of the lungs) open. Surfactant is necessary for the lungs to function properly. Without enough surfactant, a baby’s alveoli will collapse with each breath, causing the baby to work harder to breathe. If too many of the alveoli collapse, the baby might become exhausted from the work needed to breathe, which makes it even more difficult for them to breathe in the oxygen they need from the air without medical treatment.5
Signs and Symptoms5
- Breathing problems at birth that get progressively worse
- Blue skin color (cyanosis)
- Flaring nostrils
- Rapid breathing
- Grunting sounds with breathing
- Ribs and breastbone pulling in when the baby breathes (chest retractions)
What to Expect

RDS is one of the most common problems for premature babies, affecting nearly all newborns born before 28 weeks of gestation.2 This is due to the fact that a fetus begins producing surfactant at about 26 weeks of gestation; if a baby is born preterm, they might not have produced enough surfactant yet.2 Although premature babies are more likely to have RDS, a form of the condition also can affect full-term infants.
Babies will experience symptoms of RDS differently, but symptoms will typically worsen within the first few days after birth, peaking on the third day, and then will improve with medical treatment.5 Each baby’s treatment will depend on their individual needs—some will require more oxygen than others or some may need a breathing machine. As a baby’s condition improves, he or she may need less oxygen and assistance with breathing.
An RDS diagnosis can be stress inducing for a baby’s family, but it may help to know that in the majority of cases, RDS is very treatable with expert care.2,5 Most babies with RDS will be moved to a NICU, where a team of experts specializing in treating premature newborns can give the baby round-the-clock care and treatment.8 Remember that it is typical for RDS to worsen over the first 2 to 3 days.5 As your baby gets better, he or she may breathe more comfortably and may need less oxygen and support.9 Since babies with RDS also commonly have other problems associated with being born prematurely, they may continue to need care in the NICU until they are well enough to go home.
What can you expect in the NICU?
- Respiratory Distress Syndrome (RDS) in Premature Babies, default – Stanford Children’s Health. (n.d.). Stanford Children’s.
- Respiratory Distress Syndrome | NHLBI, NIH. (2019, April 9).
- Infant Respiratory Distress Syndrome (Hyaline Membrane Disease) | Boston Children’s Hospital. (n.d.). Children’s Hospital.
- Respiratory Distress Syndrome: Brighter Prospects for Premature Babies | NHLBI, NIH. (2011, August 01).
- Respiratory Distress Syndrome. (n.d.). Children’s Hospital of Philadelphia.
- Image courtesy of Dr. Mikael Häggström. Republished under the Creative Commons CC0 1.0 Universal Public Domain Dedication license.
- Image courtesy of Dr. Ian Bickle.
- Respiratory Distress Syndrome (for Parents) – Nemours KidsHealth. (n.d.). Kidshealth.
- Respiratory Distress Syndrome: Newborn. (n.d.). Nationwide Children.